Dear Sir:
In patients who experience acute stroke, excessive blood pressure (BP) lowering may result in early neurological deterioration (END) [1] and unfavorable clinical outcomes [2]. Thus, pharmacologically induced hypertension (PIH) may be effective for patients with signs of END. Although a few studies have reported potential benefits [3-7], the feasibility and safety of PIH remain unclear. We aimed to identify the characteristics of patients who require PIH therapy and to examine the feasibility, safety, and potential efficacy of PIH.
At the Asan Medical Center, we have been performing PIH therapy since 2011 for patients who exhibit END or are at increased risk for END, such as those with fluctuating neurological symptoms, based on the results from previous studies [4,5,7]. Although END was defined as an increase in National Institutes of Health Stroke Scale (NIHSS) score ≥2, patients with a 1-point increase were occasionally included according to the attending neurologist’s judgment. PIH was not performed in patients with systolic BP >180 mm Hg or diastolic BP >110 mm Hg, ventricular tachycardia, or symptomatic heart or renal failure. However, because PIH is not an established treatment, some patients with END were treated by augmenting fluid therapy without PIH according to the discretion of attending physicians. For PIH, BP elevation of 15% to 25% over baseline was targeted, with a maximum systolic BP of 220 mm Hg [3,5]. Phenylephrine (50 mg) mixed with 250 mL of normal saline was intravenously administered at a rate of 0.3 μg/kg/min and titrated every 30 to 60 minutes. PIH was usually maintained for 5 days and tapered thereafter. If END recurred, PIH was re-administered for several days.
Two groups were selected as controls: the first was matched with age and sex (CT1) and, the second, with an additional stroke subtype (CT2). Considering the expected unfavorable outcome in patients with END [8], a favorable functional outcome was defined as a modified Rankin Scale (mRS) score of ≤3 at 3 months post-stroke. “Early responsiveness” was defined when patients exhibited neurological improvement (NIHSS score ≥2 improvement or physician’s documentation for neurological improvement) within 1 day after PIH initiation. BP was recorded at four time points: the first-measured hospital BP (initial BP [iBP]); BP checked immediately before starting PIH (baseline BP [BP0]); BP checked at 7:00 AM 1 day after starting PIH (BP1); and BP checked at 7:00 AM 1 day after completing PIH (end BP [eBP]). This study was approved by the Institutional Review Board of Asan Medical Center, and the requirements for informed written consent was waived.
Between 2011 and 2016, 121 patients were treated with PIH (mean±standard deviation age, 65.9±12.7 years; women, 40%). Compared with CT1 patients, PIH patients more often had small vessel disease (SVD, 42.3% vs. 19.8%) and large artery disease (LAD, 41.3% vs. 31.4%), and less often experienced cardioembolic stroke (4.15% vs. 34.7%) (P<0.001, chi-square test). As stroke subtype may be associated with patient outcome, subsequent analyses was performed with CT2 patients. PIH patients had significantly higher systolic iBP, higher initial NIHSS score, and more often had END compared with CT2 patients (Table 1).
In the PIH group, the mean arterial pressure of BP0 (96.9±13.4 mm Hg) decreased from that of iBP (108.5±17.9 mm Hg). After PIH treatment, mean systolic BP1 (166.4±19.3 mm Hg) was elevated by 24.8%±19.3% from BP0 (135.3±18.6 mm Hg), and diastolic BP1 (83.6±13.7 mm Hg) was elevated by 9.3%±9.2% from BP0 (77.7±12.9 mm Hg). The mean PIH duration was 5.8±2.7 days. The mean time to achievement of target BP was 7.6±4.6 hours.
Nine patients developed hemorrhagic transformation—three in the PIH group and six in the CT2 group—and there were no symptomatic intracerebral hemorrhages. In the CT2 group, two patients died from cerebral herniation. Among PIH patients, five experienced sinus bradycardia and one a sinus pause, which eventually improved. One patient developed vasogenic edema, one experienced renal failure, and one pulmonary hypertension. Among the CT2 patients, one developed sinus pause, one renal failure, and one pulmonary hypertension.
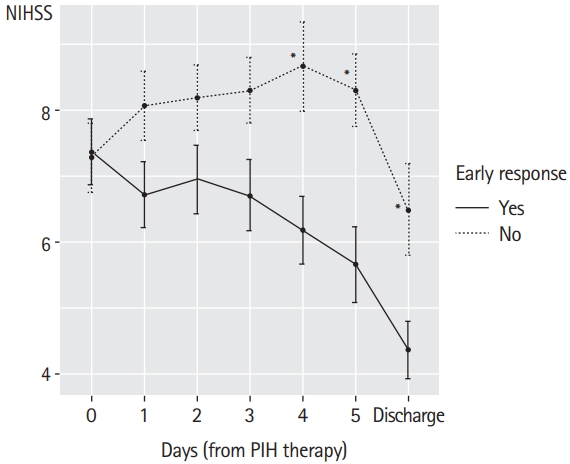
The aggravation of neurological deficit (highest NIHSS score−initial NIHSS score) was greater in PIH patients than in CT2 patients (3.7 vs. 1.0, P<0.001). PIH patients less often experienced favorable outcomes than CT2 patients at discharge but exhibited greater resolution of neurological deficit (delta NIHSS [highest NIHSS score-discharge NIHSS score]) at discharge. Of 110 patients in whom mRS was assessed at 3 months, the difference in the proportion of favorable mRS score was marginal (P=0.059) (Table 1). Fifty-four PIH patients (44.6%) exhibited “early-response,” in whom NIHSS score was significantly lower after 4 days than in those without early response (Figure 1). Their functional status was significantly better at discharge and at 3 months (Table 2), although the difference was not apparent when mRS ≤2 was used as a “favorable” outcome (P=0.276 and P=0.156, respectively).
PIH was more often performed in patients with SVD and LAD than in those with cardioembolism, which is in agreement with the observation that the pathogenesis of END in patients with LAD or SVD is associated with impaired perfusion [9,10]. Although END may also result from other mechanisms, such as edema development or hemorrhagic transformation [8], PIH did not increase the incidence of adverse effects in our patients. Thus, PIH is feasible and safe, if performed carefully.
As this was not a randomized controlled study, we were unable to evaluate the efficacy of PIH therapy. Initial neurological deficits were more severe in those with PIH than in CT2 patients, and most patients in the PIH group experienced END. However, resolution of neurological deficits (delta NIHSS) was more marked in the PIH group, and mRS scores at 3 months post-stroke did not differ between the two groups, suggesting the potential benefit of PIH therapy. Among patients receiving PIH, the final functional outcome was significantly better in early responders than in the others (Table 2 and Figure 1), suggesting that early response may predict a better final functional outcome. Although this was an uncontrolled, observational study involving a relatively small number of patients, our data suggest that PIH therapy in patients with END is feasible, safe, and potentially effective, warranting further controlled trials to confirm its efficacy.