 |
 |
- Search
| J Stroke > Volume 17(3); 2015 > Article |
|
Dear Sir:
Anticoagulation in acute ischemic stroke (AIS) is not generally recommended because of the risk of intracranial bleeding. However, patients with AIS who have concurrent left ventricular (LV) thrombus and atrial fibrillation (AF) are particularly at high risk of early recurrent embolization and thereby might require urgent anticoagulation. In this clinical scenario, compared to warfarin, non-vitamin K oral anticoagulants would be more advantageous because of their rapid onset of action, lower risk of intracranial bleeding, and lack of prothrombotic activity.
Herein, we report a case of dabigatran therapy that resolved LV thrombus in a patients with AIS and AF.
A 57 year-old man presented to the emergency room with left hemiparesis and neglect that developed 20 minutes ago. Seven months ago, he was treated with stent insertion in the proximal left anterior descending artery due to ST-elevation myocardial infarction and diagnosed with AF. Since then, he had been taking aspirin and clopidogrel. At admission, the initial National Institute of Health Stroke Scale score was 10 (best gaze 1, facial palsy 2, arm motor 1, leg motor 3, sensory 2, and neglect 1). Computed tomography angiography revealed right distal M1 occlusion. Intravenous alteplase (0.9 mg/kg) and stent-retriever thrombectomy successfully recanalized the right M1 occlusion after 2.5 hours from the onset.
Transthoracic echocardiography performed at the day of admission revealed a thrombus (11├Ś 8.9 mm) at LV apex associated with apical inferior wall akinesia. However, there was no evidence of acute myocardial infarction: no ST segment elevation in electrocardiography and normal cardiac enzyme levels except for mildly elevated troponin I (0.26 ┬Ąg/L: normal level < 0.11 ┬Ąg/L). After 24 hours, his neurological symptom substantially improved (National Institute of Health Stroke Scale score 0). Diffusion-weighted and gradient-echo images taken 24 hours after symptom onset showed multifocal ischemic changes in bilateral middle cerebral artery territories without hemorrhagic transformation. Taking into account both the necessity of and the bleeding risk with immediate anticoagulation, we started dabigatran 110 mg twice daily after 2 days of stroke onset. On follow-up transthoracic echocardiography conducted after 7 days of dabigatran treatment, LV thrombus disappeared without thromboembolic episode (Figure 1). We considered that the index stroke was caused by LV thrombus, for which short-term, 3-month anticoagulation is generally recommended. However, this patient had AF and stroke, and thereby long-term anticoagulation was required. After discharge, the dose of dabigatran was increased from 110 mg twice daily to 150 mg twice daily, and he has had neither recurrent stroke nor bleeding complication.
To the best of our knowledge, this is the first case where dabigatran safely and successfully resolved LV thrombus in a patient with AIS. Previously, several case reports illustrated that non-vitamin K oral anticoagulant treatment resolved LV thrombus associated with coronary heart disease or heart failure [1-3]. In this case, the risk of re-embolization without anticoagulation would be substantial because of the co-existence of LV thrombus and AF, but the risk of intracranial bleeding would be also high given the acute stage of ischemic stroke treated with intravenous and endovascular reperfusion therapy. Therefore, this would be the case that requires immediate, effective, and safe anticoagulation.
We might have three options for this case: warfarin alone, bridging heparin and warfarin, and non-vitamin K oral anticoagulants. Warfarin alone might have disadvantages of delayed onset of action and potential prothrombotic activity related to inhibition of protein C and protein S during the early period of warfarin initiation. In a population-based case-control study, stroke risk was paradoxically and substantially increased with warfarin therapy during the first 30-day of initiation [4]. In a recent case who had AIS associated with thrombus in the left atrial appendage and AF and was treated with warfarin alone, left atrial appendage thrombus enlarged and early recurrent embolic stroke developed [5].
To avoid initial prothrombotic status and expedite anticoagulation effect, bridging therapy with heparin or low molecular weight heparin and warfarin is generally recommended in deep vein thrombosis and LV thrombus associated with acute myocardial infarction. However, in patients with AIS due to cardioembolism, the bridging therapy increased the risk of serious bleeding [6].
Without anticoagulation, 3-month embolism risk with LV thrombus was reported to be 10% to 20% [7,8]. In contrast, the annual stroke risk with AF ranged from 1.9% to 18.2%. Before the index stroke, our patient had a risk factor of vascular disease only, which indicates that his annual stroke risk with AF would be less than 2.0% [9]. Therefore, the index stroke in this case was likely to be caused by LV thrombus rather than AF.
Dabigatran is a selective thrombin inhibitor. In contrast to warfarin, dabigatran neither inhibits protein C and protein S nor interferes tissue factor-factor VIIa complexes. Tissue factor is abundant in the perivascular system of the brain, and the tissue factor-factor VIIa complexes provide hemostatic effect in the setting of cerebrovascular injury [10]. In a large clinical trial, dabigatran compared to warfarin had a substantially lower risk of intracranial bleeding and similar or better efficacy of preventing stroke [11]. In addition, dabigatran offers anticoagulation effect within 2 hours after administration. Therefore, in patients who require a rapid, effective, and safe anticoagulation strategy, dabigatran might be a useful option. In this case, we observed a relatively rapid resolution of LV thrombus with 7 days of dabigatran therapy. However, for left atrial appendage thrombus, there have been contradictory cases of formation as well as resolution of thrombus in AF patients with dabigatran therapy [12,13]. Therefore, further research is needed to better understand the response of LV or left atrial appendage thrombus to dabigatran or other non-vitamin K oral anticoagulants.
Notes
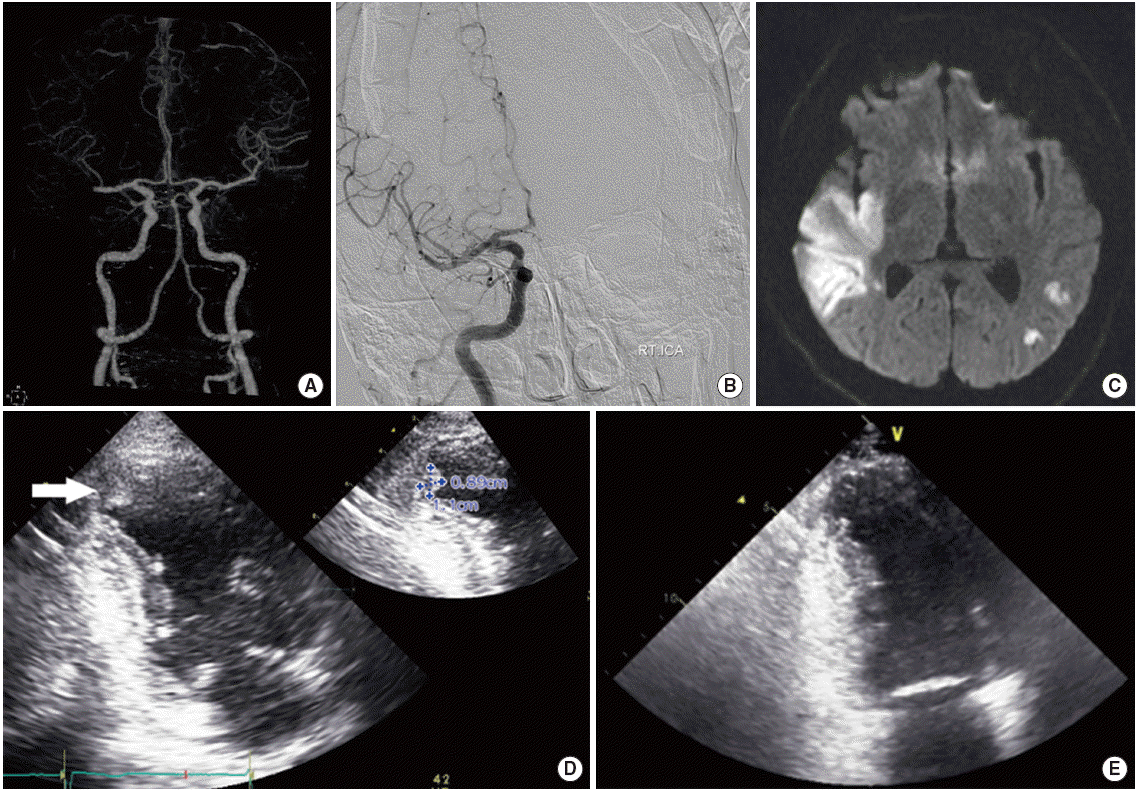
Figure┬Ā1.
(A) Right distal M1 occlusion at presentation. (B) Reperfusion after stent-retriever thrombectomy. (C) Diffusion-weighted image obtained at the next day of reperfusion therapy. (D) Left ventricular thrombus before dabigatran treatment. (E) Resolution of left ventricular thrombus after 7 days of dabigatran treatment.
References
1. Nagamoto Y, Shiomi T, Matsuura T, Okahara A, Takegami K, Mine D, et al. Resolution of a left ventricular thrombus by the thrombolytic action of dabigatran. Heart Vessels 2014;29:560-562.


2. Padilla P├®rez M, Salas Bravo D, Garcel├Īn Trigo JA, Vazquez Ruiz de Castroviejo E, Torres Llergo J, Lozano Cabezas C, et al. Resolution of left ventricular thrombus by rivaroxaban. Future Cardiol 2014;10:333-336.


3. Mano Y, Koide K, Sukegawa H, Kodaira M, Ohki T. Successful resolution of a left ventricular thrombus with apixaban treatment
following acute myocardial infarction. Heart Vessels 2014;DOI: 10.1007/s00380-014-0562-z.


4. Azoulay L, DellŌĆÖAniello S, Simon TA, Renoux C, Suissa S. Initiation of warfarin in patients with atrial fibrillation: early effects on ischaemic strokes. Eur Heart J 2014;35:1881-1887.



5. Kim Y, Bang OY. Paradoxical procoagulant effect of early doses of warfarin: possible role of non-vitamin K oral anticoagulant in patients with atrial fibrillation-related stroke. J Stroke 2015;17:216-218.



6. Hallevi H, Albright KC, Martin-Schild S, Barreto AD, Savitz SI, Escobar MA, et al. Anticoagulation after cardioembolic stroke: to bridge or not to bridge? Arch Neurol 2008;65:1169-1173.



7. Keren A, Goldberg S, Gottlieb S, Klein J, Schuger C, Medina A, et al. Natural history of left ventricular thrombi: their appearance and resolution in the posthospitalization period of acute myocardial infarction. J Am Coll Cardiol 1990;15:790-800.


8. Vaitkus PT, Barnathan ES. Embolic potential, prevention and management of mural thrombus complicating anterior myocardial infarction: a meta-analysis. J Am Coll Cardiol 1993;22:1004-1009.


9. European Heart Rhythm Association; European Association for Cardio-Thoracic Surgery, Camm AJ, Kirchhof P, Lip GY, Schotten U, Savelieva I, Ernst S, et al. Guidelines for the management of atrial fibrillation: the Task Force for the Management of Atrial Fibrillation of the European Society of Cardiology (ESC). Eur Heart J 2010;31:2369-2429.



10. Mackman N. The role of tissue factor and factor VIIa in hemostasis. Anesth Analg 2009;108:1447-1452.



11. Connolly SJ, Ezekowitz MD, Yusuf S, Eikelboom J, Oldgren J, Parekh A, et al. Dabigatran versus warfarin in patients with atrial fibrillation. N Engl J Med 2009;361:1139-1151.









