Dear Sir:
In the modern era of ischemic stroke treatment, stroke physicians have highly effective tools to recanalize occluded major cerebral arteries. After hyperacute treatments, deleterious effects of reperfusion into the ischemic brain, including oxidative injuries, extravasation of intravascular blood, and recurrent infarctions should be managed appropriately. Statins may be a feasible and effective therapeutic option because of their pleiotropic effects, such as the stabilization of endothelial activation, augmentation of cerebral blood flow, and anti-oxidative and anti-inflammatory effects protecting against ischemic-reperfusion injuries [1-3]. Several studies have attempted to evaluate therapeutic potential of statins to address this issue, but the majority of such studies analyzed the effect of statin medication before stroke or statin withdrawal after stroke [4]. Considering the early development of oxidative and inflammatory injuries after recanalization treatment, it may be better to initiate statins earlier to obtain the best effects. Previously, we reported on the efficacy of early statin use after recanalization treatment [5]. In this current study, we aimed to update the analysis with recent data on recanalization treatment and to determine the subgroups that benefit from early statin initiation (≤72 hours).
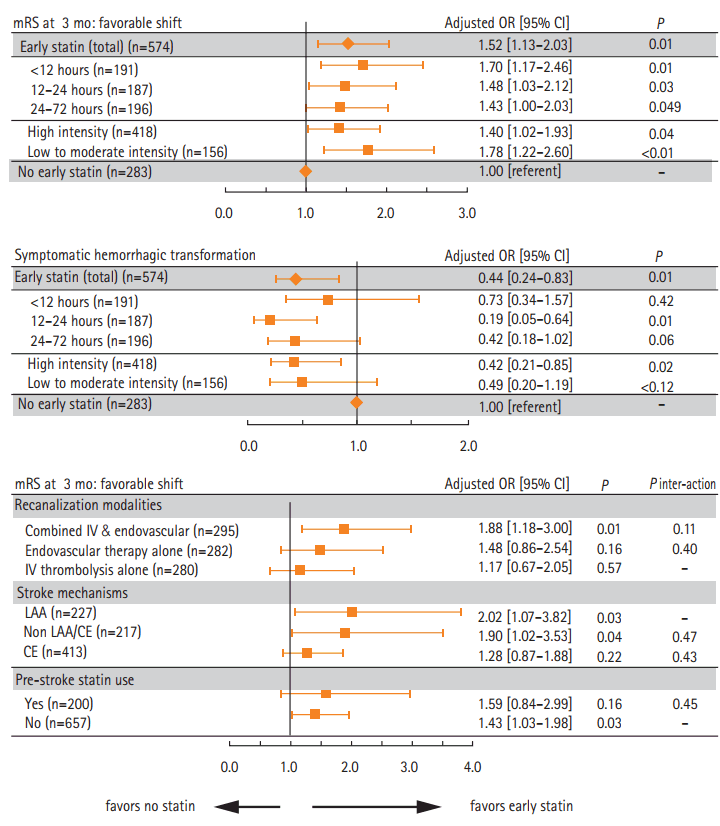
A total of 857 acute ischemic stroke patients treated with intravenous or endovascular recanalization between July 2007 and December 2015 were identified from a prospective clinical registry from a single center. We retrospectively obtained data on the timing and dose of statins from an electronic barcode medication administration system. Favorable shifts on the modified Rankin Scale score at 3 months and symptomatic hemorrhagic transformation were analyzed, and clustering effects by treatment year were considered. Early statins were used in 67% (n=574) of the patients, with 33% (n=191) receiving them within 12 hours. High-intensity statins (atorvastatin 40-80 mg or rosuvastatin 20 mg) were used in 73% (n=418) of patients, and low-to-moderate intensity statins were used in 27% (n=156) of patients (Supplementary Tables 1 and 2). Adjusted multivariable analyses revealed that early statin initiation within 72 hours was associated with a favorable modified Rankin Scale score shift (adjusted odds ratio 1.52; 95% confidence interval 1.13-2.03) compared with no statin therapy (Figure 1). Early statins were also associated with decreased odds of having symptomatic hemorrhagic transformation (adjusted odds ratio 0.44; 95% confidence interval 0.24-0.83). Early statins showed no substantial exposure-response relationship with time of initiation or intensity. The beneficial effects of early statin initiation maintained in subgroup analyses regarding the mode of recanalization, stroke mechanism, and statin use before the index stroke. The clinical profiles in the exposure-response and subgroup analyses are provided in Supplementary Tables 3-7. The full models of multivariable logistic regression analyses are presented in Supplementary Table 8.
This study shows that early initiation of statins may confer improved functional recovery and decrease hemorrhagic transformation after recanalization treatment for acute ischemic stroke, regardless of treatment modalities, stroke mechanisms, and pre-stroke statin use. Several studies have reported the efficacy of early statin use after recanalization treatment, but they included only intravenous thrombolysis cases [6] or were mostly performed before stent-retrievers were used in a majority of patients [5,7]. In addition, the post-treatment National Institute of Health Stroke Scale score was incorporated into all models in our study as a covariate, which resulted in more accurate assessment of the effect of early statins following recanalization treatment [8].